Key details
- High prevalence of injury: Acute radiation dermatitis affects up to 95% of patients undergoing radiotherapy, representing a substantial unmet clinical need.[1]
- Investigational treatment: A Phase II clinical trial has evaluated a hydrogel containing placental mesenchymal stem cells (PMSCs) for the management of radiation-induced skin injury.[2]
- Observed clinical effect: Wound deterioration occurred in 8% of patients receiving PMSC hydrogel compared with 50% in the control group treated with standard hydrogel.[2]
What is radiation-induced skin damage?
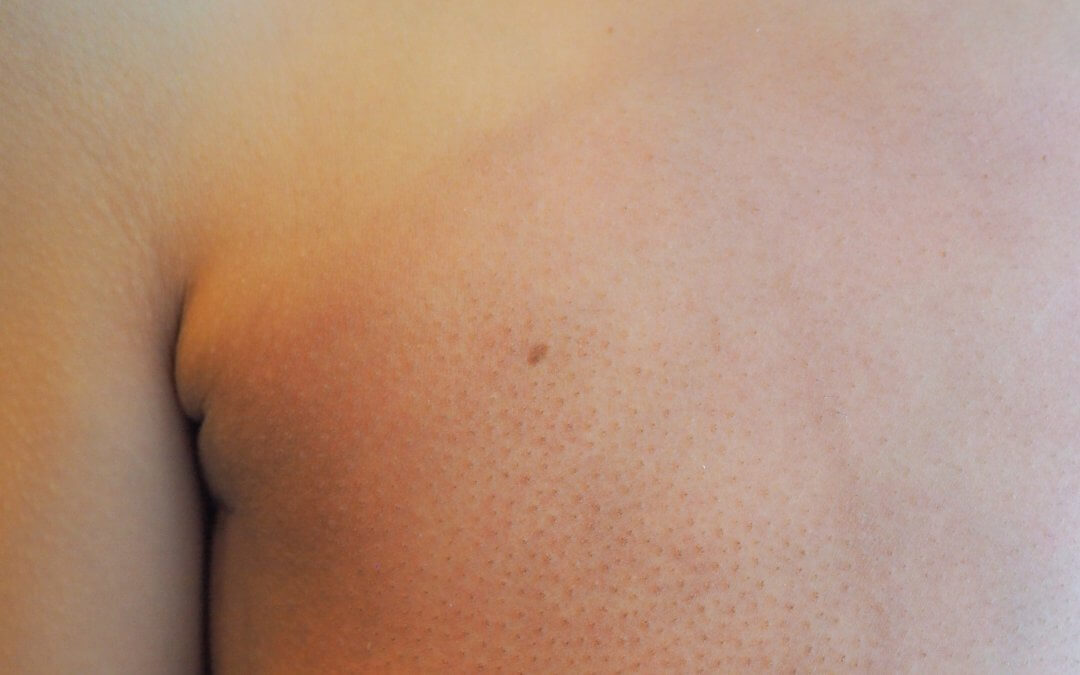
Radiation-induced skin damage (radiodermatitis) is a common negative side effect of radiotherapy. The radiation affects skin cells, causing DNA damage and reducing the skin’s ability to heal.[1]
- Prevalence: Up to 95% of patients receiving radiotherapy experience some degree of skin injury.[1]
- Clinical presentation: Symptoms range from mild redness to painful skin peeling and weeping (moist desquamation), ulceration, and necrosis.[2]
- Disease course: The condition typically worsens with cumulative radiation dose and with longer radiation treatment duration, particularly in areas where tissue is shallow or the cancer being treated is closer to the skin.[1][3]
- Healing characteristics: Compared to other skin injuries, these wounds often last longer and heal slower.[1][3]
Despite its high frequency and its potential to negatively affect quality of life and even interrupt cancer treatment, there is currently no universally accepted standard of care beyond supportive skin and wound care strategies.[1][3] Advances in medication and the development of biomaterial-based dressings, including hydrogels, have shown potential to improve outcomes; however, effectiveness remains variable and further validation is needed.[4][5]
Rationale for PMSC hydrogel
Placental mesenchymal stem cells (PMSCs) have been investigated for their regenerative and immunomodulatory properties. When delivered via a hydrogel matrix, these cells may provide:
- Localised delivery to the wound environment
- Potential modulation of inflammation
- Support for tissue repair
This approach remains investigational, and its clinical utility is under evaluation.[2]
What were the results of the clinical trial?
A Phase II double-blind, randomised controlled trial assessed the efficacy and safety of a PMSC-embedded hydrogel in patients with moderate-to-severe radiation-induced skin injury.[2]
Trial structure:
- 66 participants with grade 2 or higher radiodermatitis
- 44 patients randomly assigned to receive PMSC hydrogel; the remaining 22 received normal hydrogel
- Once-daily application for 6 consecutive days
- The study was double-blinded, meaning neither patients nor the doctors applying the treatment knew who was receiving the active gel
Key outcomes:
- Wound progression: A lower proportion of patients in the treatment group experienced wound worsening (8%) compared with the control group (50%).[2]
- Pain outcomes: A greater reduction in patient-reported pain was observed in the treatment group.[2]
- Healing endpoints: Although complete healing rates did not differ significantly within the 15-day observation period, the trend favoured the PMSC treatment group.[2]
The authors note that the short follow-up period may have limited interpretation of longer-term healing outcomes and recommend further evaluation in larger Phase III studies.[2]
Broader research into placental-derived therapies
Placental tissues, including amniotic membrane and placental derived-stem cells, are being investigated across multiple clinical applications due to their biological properties.[6][7]
Current areas of research and use include:
- Ophthalmology: Amniotic membrane grafts are used in the management of eye disorders and injuries.[8][9]
- Wound care: Applications in chronic wounds, including diabetic foot ulcers and reconstructive procedures.[10][11]
- Chronic conditions: Ongoing clinical trials are evaluating placental-derived stem cells in conditions such as multiple sclerosis[12] and osteoarthritis.[13]
While early findings are promising, most applications remain under clinical investigation, and further high-quality evidence is needed to establish efficacy, safety, and appropriate clinical use.
If you would like to learn more about stem cells, including current research and how they may be used in medicine, you can request our free guide for general information.
References
[1] Behroozian T, Goldshtein D, Ryan Wolf J, van den Hurk C, Finkelstein S, Lam H, Patel P, Kanee L, Lee SF, Chan AW, Wong HCY, Caini S, Mahal S, Kennedy S, Chow E, Bonomo P; MASCC Oncodermatology Study Group Radiation Dermatitis Guidelines Working Group. MASCC clinical practice guidelines for the prevention and management of acute radiation dermatitis: part 1) systematic review. EClinicalMedicine. 2023;58:101886. doi:10.1016/j.eclinm.2023.101886.
[2] Tian L, et al. Topical application of a placental mesenchymal stem cell-embedded biomaterial hydrogel accelerates repair of radiation-induced skin damage: a double-blind randomised Phase II clinical trial. Journal of Translational Medicine. 2025;23:1057. doi:10.1186/s12967-025-07060-7.
[3] Yang X, Ren H, Guo X, Hu C, Fu J. Radiation-induced skin injury: pathogenesis, treatment, and management. Aging (Albany NY). 2020 Nov 16;12(22):23379-23393. doi: 10.18632/aging.103932. Epub 2020 Nov 16. PMID: 33202382; PMCID: PMC7746368.
[4] Liu Y, Xu J, Yang S, Song S, Zhao S, Dang Y. Advances in the prevention and treatment of radiation skin injury: mechanisms, pharmacological interventions, and applications of novel dressings. International Journal of Nanomedicine. 2026;21:572134. doi:10.2147/IJN.S572134.
[5] Su Y, Cui H, Yang C, Li L, Xu F, Gao J, Zhang W. Hydrogels for the treatment of radiation-induced skin and mucosa damages: an up-to-date overview. Frontiers in Materials. 2022;9:1018815. doi:10.3389/fmats.2022.1018815.
[6] Parolini O, et al. Concise review: isolation and characterisation of cells from human term placenta: outcome of the first international workshop on placenta-derived stem cells. Stem Cells. 2008;26(2):300–311. doi:10.1634/stemcells.2007-0594.
[7] S.Moonshi, H.Adelnia, Y.Wu, H. T.Ta, Placenta-Derived Mesenchymal Stem Cells for Treatment of Diseases: A Clinically Relevant Source. Adv. Therap.2022, 5, 2200054. doi:https://doi.org/10.1186/s12967-025-07060-7
[8] Mancini M, Palino P, Valastro A, Scolaro A, Oliverio GW, Mancini A, Aragona P, Meduri A. Sutureless Amniotic Membrane Grafting in the Management of Corneal Perforations Associated with Severe Ocular Surface Disease. Clin Ophthalmol. 2026 Feb 26;20:571757. doi: 10.2147/OPTH.S571757. PMID: 41777855; PMCID: PMC12951867.
[9] Daryabari SH, Ghasemian M, Lotfi E, Solouki A, Lin K, Manoochehrabadi T, Hosseini Imeni SM, Esmaeili Gouvarchin Ghaleh H. Placental-Derived Products for Corneal Regeneration: Applications of Amniotic Membrane, Cord Blood Serum, and Stem Cells: A Review. Transplant Cell Ther. 2026 Jan;32(1):13-45. doi: 10.1016/j.jtct.2025.09.024. Epub 2025 Sep 17. PMID: 40972961.
[10] Ruiz-Muñoz M, Martinez-Barrios FJ, Lopezosa-Reca E. Placenta-derived biomaterials vs. standard care in chronic diabetic foot ulcer healing: A systematic review and meta-analysis. Diabetes Metab Syndr. 2025 Jan;19(1):103170. doi:10.1016/j.dsx.2024.103170. Epub 2024 Dec 10. PMID: 39689387.
[11] Yang C, Xiong AB, He XC, Ding XB, Tian XL, Li Y, Yan H. Efficacy and feasibility of amniotic membrane for the treatment of burn wounds: A meta-analysis. J Trauma Acute Care Surg. 2021 Apr 1;90(4):744-755. doi: 10.1097/TA.0000000000003050. PMID: 33284236.
[12] Shokati, A., Nikbakht, M., Sahraian, M.A. et al. Cell therapy with placenta-derived mesenchymal stem cells for secondary progressive multiple sclerosis patients in a phase 1 clinical trial. Sci Rep 15, 16005 (2025). https://doi.org/10.1038/s41598-025-00590-6
[13] Khalifeh Soltani S, Forogh B, Ahmadbeigi N, Hadizadeh Kharazi H, Fallahzadeh K, Kashani L, Karami M, Kheyrollah Y, Vasei M. Safety and efficacy of allogenic placental mesenchymal stem cells for treating knee osteoarthritis: a pilot study. Cytotherapy. 2019 Jan;21(1):54-63. doi: 10.1016/j.jcyt.2018.11.003. Epub 2018 Dec 3. PMID: 30522806.
FIND OUT MORE, REQUEST YOUR WELCOME PACK TODAY
All you need to know to make an informed decision.
Provide your contact details to request:
– Complete Welcome Pack and Parent’s Guide
– Information via email
– Contact from our specialist advisors

Lesley-Ann Martin, PhD
Chief Scientific Officer at Cells4Life
Dr. Martin holds a PhD in Molecular Biology from the University of Reading and has extensive research experience at the Institute of Cancer Research. She oversees all scientific and laboratory operations at Cells4Life.