In early July 2017 a panel of cancer experts unanimously endorsed CAR-T treatment for leukaemia. With FDA approval expected, it will become the first gene therapy to reach the market creating a ‘living drug’ that genetically alters a patients own cells to fight cancer.
Phase-2 Trials of the CAR-T reported complete remissions in 82% of patients, however, a concern was raised with the high incidence of the dangerous inflammatory condition – cytokine release syndrome
But what role does cord blood play?
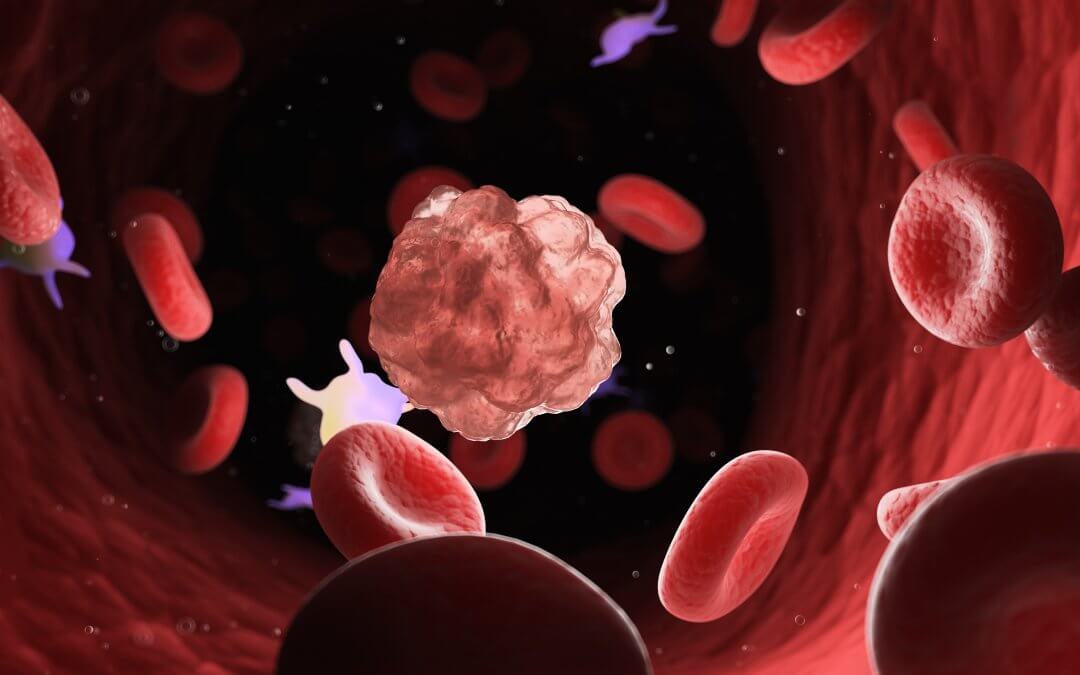
At the University of Texas M.D Anderson Cancer Centre, researchers have been looking at the role umbilical cord blood can play in this novel treatment. Scientists have discovered that natural killer cells (NK) found in cord blood can be genetically modified to hunt down and kill leukaemia and lymphoma.
Furthermore, they have found that the engineered NK cells taken from cord blood were actually more efficient at killing chronic lymphocytic leukaemia than NK cells taken from a patient’s own blood in CAR-T. The NK cells derived from cord-blood also do not need to be matched, eliminating the risk of graft vs. host disease.
M.D.Anderson continue to test cord blood derived NK cells in a phase i/ii trials asa therapy for patients with chronic lymphocytic leukaemia (CLL), acute lympocytic leukaemia (ALL) and non-hodgkin lymphoma.
Reference:
Fierce Biotech
Benefits of NK cells from cord blood:
- More efficient at killing leukaemia than cells from a patients own blood
- No matching requirements – eliminating the risk of graft vs. host disease
- Built in ‘suicide gene’ to shut down the cell if it triggers cytokine release syndrome

Request a Welcome Pack
Find out more about cord blood banking by downloading a Welcome Pack now.