Medical regulators in the UK have approved a gene-editing treatment involving bone marrow stem cells designed to cure two blood diseases, including sickle cell disease, in what is a world first.
The therapy, called Casgevy, has been given the green light by the Medicines and Healthcare products Regulatory Agency (MHRA) to treat sickle cell disease and beta thalassemia, two painful blood conditions. [1]
It is the first medicine anywhere to make use of the gene-editing tool, CRISPR, for which its inventors won the Nobel Prize in chemistry in 2020.
For people suffering from sickle cell and beta thalassemia, both inherited blood conditions triggered by defects in the haemoglobin gene, the therapy is hugely promising.
What is sickle cell disease?
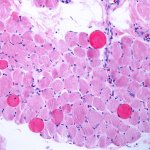
Where normal red blood cells are usually shaped like biconcave disks, making them flexible enough to move easily through blood vessels, people with sickle cell disease produce crescent or ‘sickle’ shaped red blood cells.
These misshapen red blood cells cannot bend or move easily, resulting in painful blood vessel blockages and life-threatening infections. About 17,500 people in the UK suffer from the disease. [2]
What is beta thalassemia?
People who have beta thalassemia struggle to produce enough haemoglobin, a protein used by the red blood cell to carry oxygen around the body. For sufferers of the condition, beta thalassemia can lead to severe anaemia, leaving them requiring regular blood transfusions, injections and medicine throughout their lives. [3]
How does Casgevy work?
The therapy works by taking stem cells from a patient’s bone marrow and editing them in a lab, using the gene-editing technology CRISPR’s “genetic-scissors”. These stem cells, now treated, are then returned to the patient through infusion.
Following the infusion, patients must spend around a month in hospital while the treated cells take residence in the bone marrow. During this time the edited stem cells will begin to produce red blood cells with the stable form of haemoglobin.
In clinical trials, the new therapy was shown to eradicate severe pain in 28 of 29 patients with sickle cell treated and removed the need for blood transfusions for at least a year in 39 of the 42 beta thalassemia sufferers treated. [4]
How safe is the treatment?
Although participants experienced side effects ranging from nausea, fever and an increased risk of infection, no significant safety concerns were raised.
The manufacturer of the therapy, Vertex Pharmaceuticals and the MHRA are expected to release further results about the treatment’s safety and side-effects in due course. [5]
What does this mean if I want to store my baby’s stem cells?
If it’s likely your baby could have sickle cell disease or beta thalassemia, it may be worth considering banking their umbilical cord blood. This is because umbilical cord blood is rich in powerful stem cells which could potentially be used in a variety of therapies and treatments.
Giving your baby the gift of stem cell storage may mean that they’ll one day be able to use their cord blood stem cells for the Casgevy therapy instead of the more intrusively procured bone marrow stem cells. While not currently an approved version of the procedure, using the stem cells from banked umbilical cord blood rather than bone marrow could potentially make for a less invasive procedure overall for your child, should it become a possibility.
To find out more about how banking your baby’s stem cells may help prepare them for the future of medicine, request your free welcome pack below.
Sources
[1] https://www.gov.uk/government/news/mhra-authorises-world-first-gene-therapy-that-aims-to-cure-sickle-cell-disease-and-transfusion-dependent-thalassemia
[2] http://www.sicklecellsociety.org/about-sickle-cell/
[3] https://www.nhs.uk/conditions/thalassaemia/
[4] https://www.nature.com/articles/d41586-023-03590-6
[5] https://www.nature.com/articles/d41586-023-03590-6
FIND OUT MORE, REQUEST YOUR WELCOME PACK TODAY
All you need to know to make an informed decision.
Provide your contact details to request:
– Complete Welcome Pack and Parent’s Guide
– Information via email
– Contact from our specialist advisors